 
Studies examining determinants of vaccination decision-making have resulted in several proposed models of acceptance and resistance, most focusing on parental decision-making. Trust placed in the system that delivers vaccines, in the health professionals who recommend and administer the vaccines, in the policy-makers who decide about vaccination programs and in the different types of information about vaccines conveyed in the media also mediates the impact of these factors on vaccine hesitancy. Vaccine hesitancy is also the result of broader influences and should always be looked at in the historical, political and socio-cultural context in which vaccination occurs. 21 As we will discuss in this review, this model illustrates that vaccine hesitancy is an individual behavior influenced by a range of factors, such as knowledge or past experiences. This model was adapted from a schema summary of discussions held during a workshop on the cultural and religious roots of vaccine hesitancy in Canada in which some 40 experts from various fields (social sciences, humanities, public health, biomedical sciences) met to share their views on vaccine hesitancy in the Canadian context. 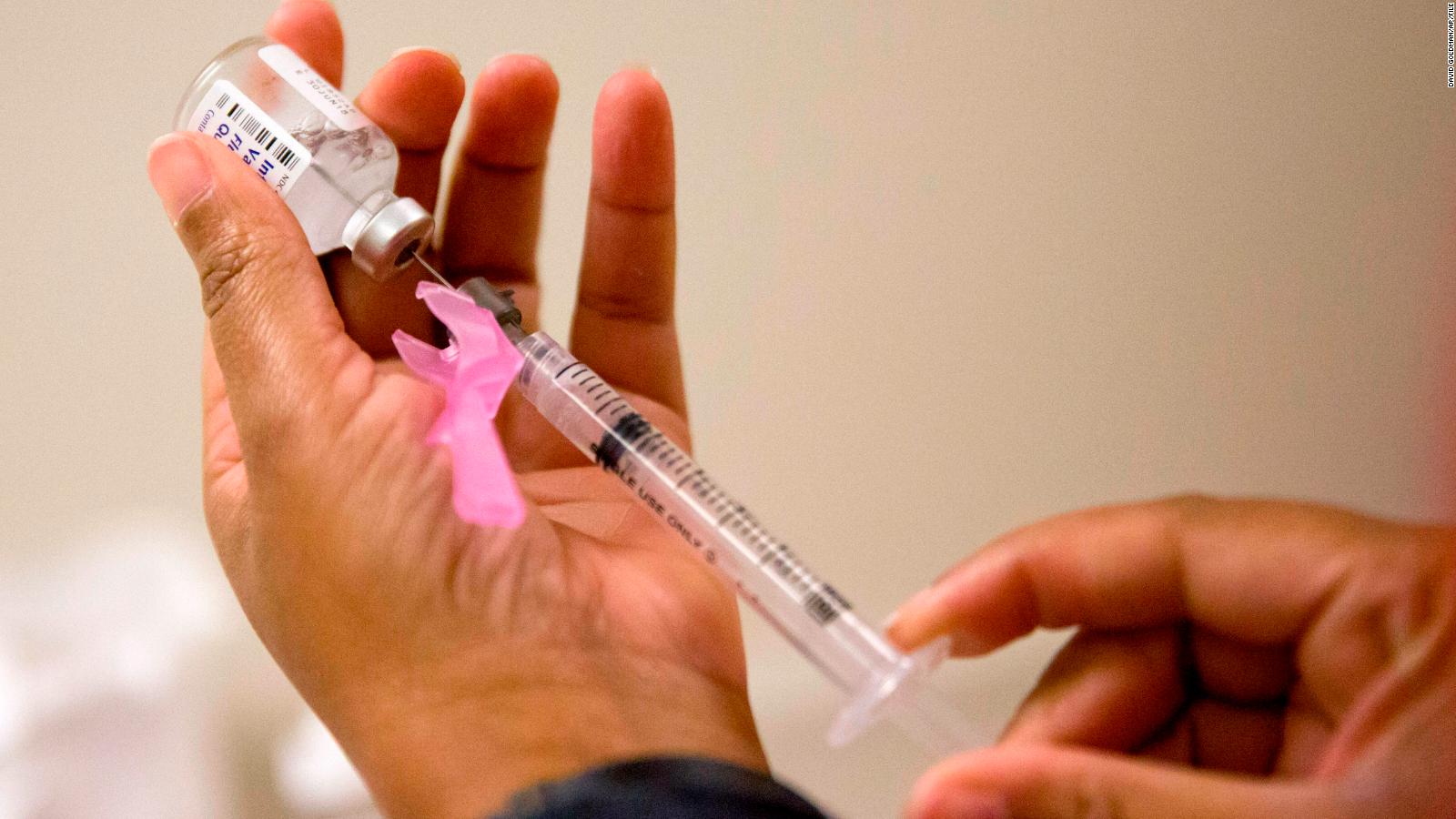
This model consists of 3 domains of factors that interact and could lead to vaccine hesitancy at the individual level. 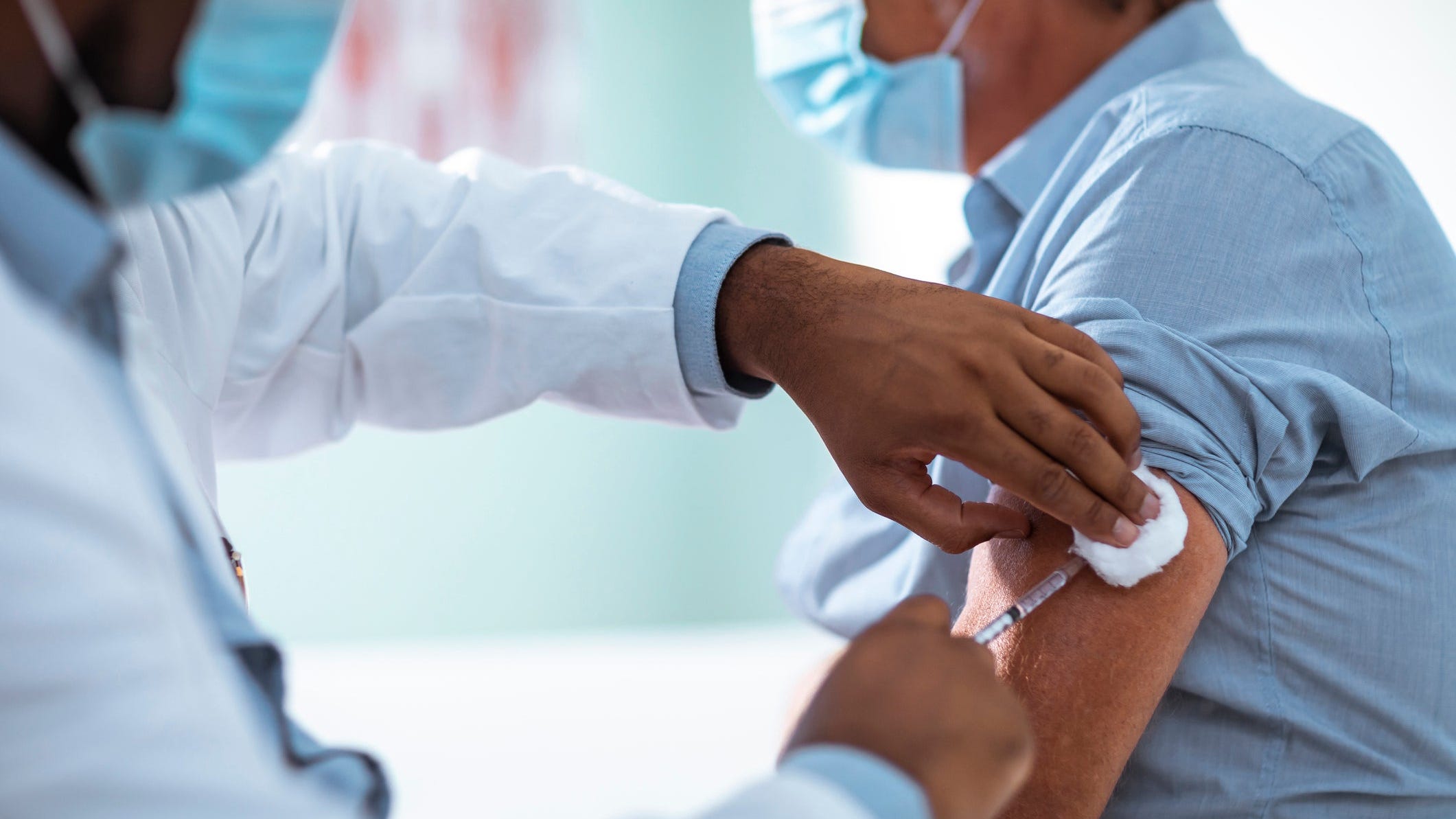
15, 16, 19 Then, we will look at determinants of individual decision-making regarding vaccination and try to synthesize the wealth of data already published on factors influencing vaccine acceptance.įigure 1 presents a conceptual model that has framed this review. 20 In this review, we will define vaccine hesitancy and look at the potential causes and determinants of the apparent increase in vaccine hesitancy in the developed world. 19 However, a more significant proportion could be categorized as being hesitant regarding vaccination. 15 - 18 It is estimated that less than 5–10% of individuals have strong anti-vaccination convictions. 14 Indeed, many experts consider that vaccination programs are threatened by growing concerns among the population regarding the safety and usefulness of vaccines. 10 - 13 For instance, in a recent pan-Canadian survey, half of the parents were concerned that new vaccines are not as safe as older vaccines and one-third felt that children today receive too many vaccines, even if nine out of ten of these parents indicated their child’s vaccination was up to date. 9 In addition, results of many studies have shown that even vaccinated individuals can have important doubts and concerns regarding vaccination. 4 Indeed, recent outbreaks of VPD, including measles, 5, 6 poliomyelitis, 7 and pertussis 8 in several parts of the developed world have been linked mainly to under-vaccinated or non-vaccinated communities. 3 However, these national estimates may hide clusters of under-vaccinated individuals. The high rate of childhood vaccination coverage in most developed countries indicates that vaccination remains a widely accepted public health measure. In addition to direct protection for vaccinated individuals, high vaccination coverage rates induce indirect protection for the overall community, or herd immunity, by slowing transmission of VPD, thereby decreasing the risk of infection among those who remain susceptible in the community. 
1 To be successful in reducing the prevalence and incidence of vaccine-preventable diseases (VPD), vaccination programs rely on a high uptake level. Vaccination programs have contributed to the decline in mortality and morbidity of various infectious diseases, and are credited with the elimination of poliomyelitis in the Americas and the worldwide eradication of smallpox. Vaccination is considered to be one of the greatest achievements of public health. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
